World AIDS Day 2023:
20 Years of MSF's work in Conakry, Guinea
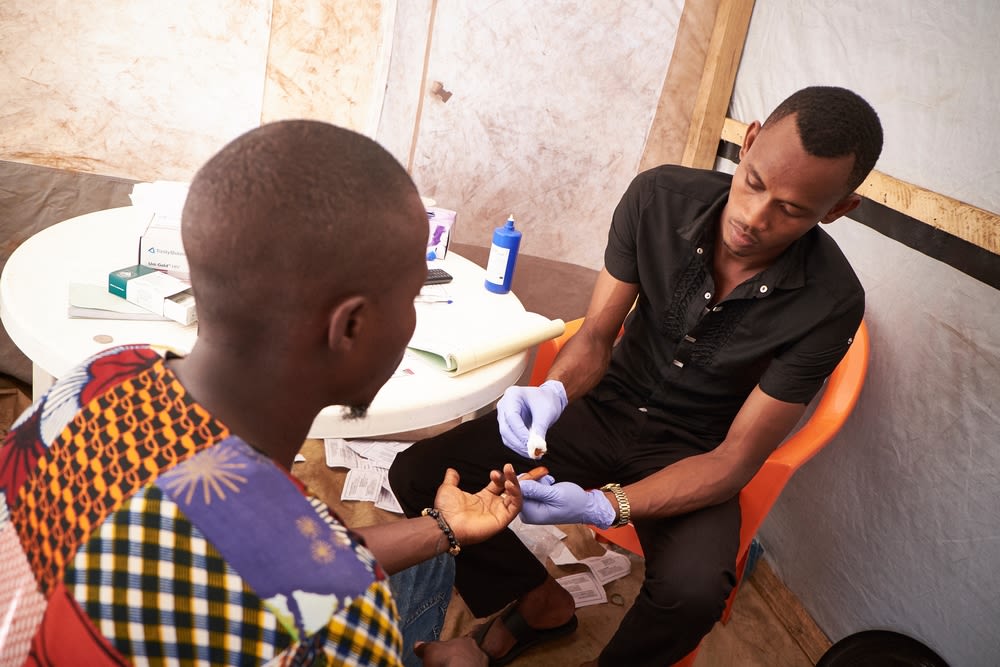
2023 marks 20 years since the opening of MSF’s HIV project in Conakry, the capital of Guinea.

Over the past two decades, MSF has been a key driving force behind implementing new medical approaches, mobilising civil society and setting up innovative distribution schemes for antiretroviral drugs

While also constantly pushing authorities and donors to increase their efforts to support HIV care in Guinea

In 2003, Guinea was not an obvious choice of location to open an HIV/AIDS project. In contrast to countries in the epicentre of the pandemic, like those in Southern Africa, where up to one in four adults were living with HIV, just 1.7%1 of Guineans were HIV-positive.
This low prevalence meant that HIV/AIDS treatment and care was not prioritised among people’s other health needs, and as a result, access to treatment was limited.
Due to the cost and the difficulty of getting hold of ARVs, some patients went on and off treatment and, as a result, developed resistance to the first-line medications, making it even more difficult to find an effective treatment regimen.
Aboubacar Camara, an MSF community educator, who is also living with HIV, says: "At some point, my treatment wasn’t well-tailored anymore. I would stop and start. I developed a resistance to the treatment. So, we had to adapt to it."
In 2004, MSF became the first organisation to provide ARVs free of charge for HIV patients in Guinea, three years before they were made available for free countrywide
Over the next decade, the number of HIV patients receiving treatment grew rapidly. Today, MSF provides care for 16,425 HIV patients, which represents 20% of the 86,000 patients on treatment countrywide.
Get to know some of the MSF patients in Guinea living with HIV

Kadiatou Bodié Baldé
I was married at the age of 13 and my husband passed away some time after. For 10 years, I was sick, but I didn’t know what was causing it. No one talked about HIV back then.
Later I remarried and discovered I was HIV positive. When my husband found out my diagnosis, he left me and my children.
I found MSF, I found a doctor, and I found community-based organisations (CBOs) that helped me get treatment. The support I received from MSF, from my friends and from CBOs saved me from feeling traumatised. I found a job and I was able to care for my children.
Once again, I remarried and both my children were born HIV negative, thanks to the prevention of mother to child transmission programme (PMTCT). Today, they are 9 and 13. My daughter knows I’m HIV-positive and has become my confidante. I told her everything, to avoid the shock of her finding out the truth from someone else. She’s the one who reminds me to take my medication. I also told her to avoid touching my blood if I were to cut myself.
MSF supported me and never gave up on me. I realised I could do something with my life and give back to the community. Today I’m proud to help people, to bring them hope and self-esteem and help them find their path. I want to thank MSF for what it has done for the people of Guinea over the past two decades. I hope that state authorities will make MSF’s expertise their own, because MSF is the gold standard and the lead to follow”.


Hassimiou Camara
I was a train conductor in 2005 when my boss called me into his office to fire me because I was off sick all the time. He suspected I had AIDS. He left the door and windows open when he made his announcement. He let me go after 24 years of service. I was livid.
A short time after, I saw an MSF commercial on television about HIV care. I went to get tested and when I got the results back, I was shocked: positive! At the time, HIV meant death. But I started my treatment and six months later I was healthy again.
Stigmatising against HIV patients is strong in Guinea. The neighbourhood kids used to come to my house to watch TV. One eventually told me that the adults had discouraged them from visiting me because I had HIV. But I don’t condemn those who stigmatise it’s the result of misinformation.
Some patients fear telling their families and communities. Some women don’t tell their partners about their diagnosis, for fear of being beaten. But those same husbands need to understand that marriage is for better or for worse, in sickness and in health. And sometimes, children abandon their parents.
I joined the Guinea Hope Foundation and in 2007 I volunteered to speak out openly. I fight to defend the sick, give them hope and courage. I help those who are afraid of HIV. I raise awareness and I am proud to lead the change. Today, stigma has decreased, and many things have changed.
In 2002, my husband and I were watching TV when a commercial came on inviting people to get screened for HIV. My husband suggested we go. As we were newlyweds, I was proud, and we went. It turned out that I was HIV positive, and my husband was HIV negative. I thought I was going to die, that my life no longer had any purpose.
One year later, we got tested again, this time by MSF. The results were the same. The major difference was that MSF gave me advice on how to live and how to accept the illness. I decided I would live positively, and MSF supported me in doing that.
After a time, my husband told his parents that I had HIV. That was when the stigma began. As I didn’t have children, my in-laws wanted my husband to get married to a second wife. But the fact I was unable to have children wasn’t because of HIV. My husband didn’t leave me. We are still together, and he remains HIV negative to this day.
I’ve volunteered for the organisation “Les amis de la santé.” I’ve also been a member of other groups for people who are HIV-positive, I’ve taken part in training sessions, and I’ve been involved. In 2010, MSF recruited me as “peer educator” to talk to the media and to encourage people to get tested. Today, I help people get married and gain acceptance from their families despite their illness.
I think it’s important to talk about HIV openly to avoid stigmatisation. For me, HIV is no different from diabetes or hypertension. If you follow your treatment regimen, you’ll live a long life. It isn’t written on our foreheads that we have HIV; people can live with it.

