New findings: a game changer for diabetes care in refugee settings
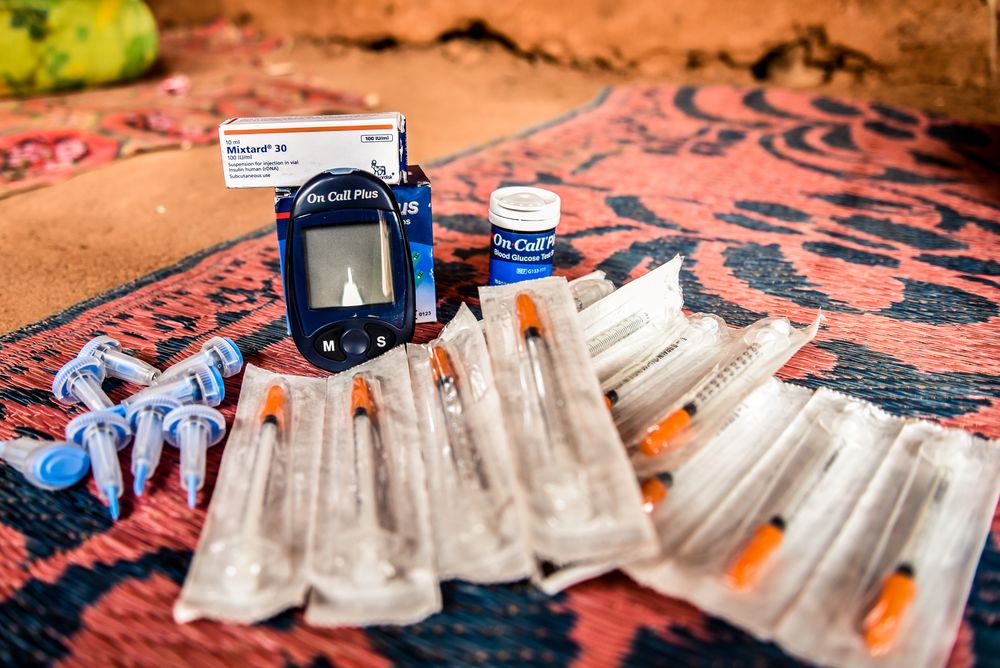
Seeking to explore ways to improve diabetes care in resource poor settings a joint study by Médecins Sans Frontières /Doctors Without Borders (MSF) and University of Geneva published today in PLOS ONE , has demonstrated that a range of insulins can be stored at temperatures ranging between 25-37 degrees for a four–week period of use.
This study confirms the possibility for people living with diabetes in similar temperature conditions to be able to use insulin, for a period of up to four weeks, even in the absence of access to refrigeration.






Diabetes is a chronic, progressive disease that can be controlled with effective treatment. However, in many countries, people living with diabetes are not getting the treatment they need to stay healthy and alive.
It is a shameful fact that only about half of people requiring insulin have access to it. Access to insulin has been largely prevented due to high prices, challenging storage requirements and complex treatment protocols.
Strict storage recommendations for insulin are difficult to follow in tropical regions and even more challenging in conflict and humanitarian emergency settings, adding an extra burden for people managing their diabetes.

Storage recommendations for insulin require refrigeration until its expiry date, or until it is opened for use.

Once in use, the storage recommendations on the label of most human insulins are below 25°C for 42 days.

In many settings, this results in people being asked to travel to the health clinic for injections and monitoring, at least twice a day, for life.

MSF works in over 70 countries worldwide and in most of these settings, insulin is often not available in public health facilities or private pharmacies.
MSF has been engaged in providing treatment for diabetes care in multiple projects across number of countries (including Jordan, Lebanon, Iraq, Syria, South Sudan, Democratic Republic of Congo, Tanzania, Kenya, Zimbabwe, and Bangladesh) to people living in resource limited and humanitarian settings.
"For far too long, we were unable to send people with diabetes back to their homes with insulin due to its cold storage requirements. Some of these people were travelling long distances daily and some even relocated to get their insulin injections at the clinic."
"With this new finding of no refrigeration requirement in a climate of up to 37 degrees and with a well-developed patient education and support programme, people with diabetes in resource limited and humanitarian settings will now be able to inject themselves in their homes greatly improving the significant disruption to their lives from having to attend hospital for twice-daily injections."


"The ability to self-inject insulin is a fundamental aspect of diabetes self-management and the ability of people with diabetes to be empowered for their health."
"We now call for a consensus statement endorsed by the World Health Organization (WHO) to support the use of locally produced cooling devices for the home storage of insulin in order to dispel the notion that refrigeration is needed in every situation."


"It is time to ensure that everyone who needs insulin, regardless of where they live, can access it. For too many people living with diabetes, life is difficult enough without this burden.”
Philippa Boulle, Non-Communicable Diseases Advisor, MSF


Watch video below to hear Philippa Boulle, Non-Communicable Diseases Advisor for MSF, speak about how these new findings can give patients with diabetes their entitlement back in terms of the right to inject their own insulin and lead a more normal life with diabetes.
PATIENTS UNDER HOME-BASED INSULIN MANAGEMENT
Mohamed Hussein Bule, 27
Mohamed is well dressed and speaks fluent English. He is a teacher in a primary school in Dagahaley, where he teaches science to the two highest classes.
Mohamed was keen on football but had to stop playing when his health suddenly deteriorated. “I used to play soccer, but I stopped in 2014 as I would get exhausted,” he says. “I started passing urine frequently and lost weight, going from 68 kg to 35 kg.”
While visiting an uncle in Nairobi in 2016, he went to a health facility where his blood sugar was tested and found to be high. He was provided with insulin, paid for by his uncle, which he took three times a day. One month later, he returned to Dadaab and came to MSF’s Dagahaley hospital.
“I went to the hospital and my treatment was changed,” he says. “Said [the former supervisor of MSF’s home-based insulin management programme] was good. He trained me a lot to be how I am today. I don’t even feel like I am diabetic. He taught me how to inject, how to understand hyper and hypoglycemia. I always wish him a successful life in future.”

Mohamed injects himself with insulin twice a day and has a follow-up visit at the hospital every three weeks. “The doctor here plans the schedules for us,” he says. “Myself I go for review every 21 days, when they also replenish our supplies. The insulin in the bottle is usually enough for 21 days.”
Mohamed says the portable cooling box is even better than the refrigerator he used before. “When you use a refrigerator, sometimes it gets too cold, so that when you inject it makes you cringe a bit,” he says. “I carry mine even to class and it does not bother anyone. People know that diabetes is not contagious, and if something can’t be transmitted, then people don’t get too concerned.”
The main challenge of the regimen, says Mohamed, is that he can’t eat for at least 30 minutes after taking insulin.

Mohamed has no problems using the glucometer. “Interpreting glucometer results is quite easy,” he says. “It works very fast and makes a beep when it’s ready. I know what range is supposed to be high or low.” Occasionally he experiences hypoglycaemia, or low blood sugar, but he has developed strategies to deal with it. “The last time I experienced it was during Ramadan, when we usually fast,” he says. “It also happens when I travel or when I walk for too long. The best way is to carry sweets in the pocket, but only eat them when you feel hypoglycaemia kicking in.”
Being a refugee presents many challenges, says Mohamed, but life in Dadaab has improved in some ways since he was a child. “When you’re a refugee, you can’t get everything you need,” he says. “When I was a child, life was difficult, but the camp has really developed over time, even the market. Travel is also difficult as movement is restricted. I find it quite difficult when I have to go to the university for my classes.”






PATIENTS UNDER HOME-BASED INSULIN MANAGEMENT
Abdirahman Ali Diyat, 4 and Abdullahi Ali Diyat, 2
Fatuma Bare Hussein is a mother of two vibrant young boys: four-year-old Abdirahman Ali Diyat, and two-year-old Abdullahi Ali Diyat. What stands out about her story is that she is fully healthy, but her two little boys both live with diabetes.
Abdirahman – Abdi, as they call him – was diagnosed with diabetes when he was nine months old. “He used to pass urine a lot and would look weak most of the time,” says Fatuma.
“I took him to the nearby health post, where we were given some syrup to give him. But when he started losing weight, I took him back to the health post. They conducted a random blood sugar test and found that his blood glucose was too high. They asked if anyone in my family had diabetes, but there’s none that I know of. I thought only old people got diabetes, not children this young.”

When her second son was born, Fatuma recognised the signs. “For the younger one, I also saw similar symptoms,” she remembers. “I couldn’t believe it. How could it be? When Abdi was diagnosed, I felt stressed, knowing he’d have to take insulin for the rest of his life. When this little one was also diagnosed, I almost gave up. I cried.”
Fatuma says her life has not been normal since Abdi was diagnosed with diabetes, and it got even more abnormal when Abdullahi had the same diagnosis.
“These are kids – they don’t know the seriousness of their condition,” she says. “Sometimes when it’s time to inject them, they run and I have to chase after them. Then they’re difficult to restrain when they see the syringe. At times you find some insulin remains in the syringe and you have to inject it into them. You know, with babies it’s very difficult to know how they are feeling – they may not be able to express the discomfort they are in. They used to cry a lot. Sometimes the sugar is low, sometimes it’s high – it’s difficult to know. The youngest one is the most difficult to handle. The four-year-old started [insulin injections] a while back and is already used to it; he thinks it’s a daily routine. My biggest fear is controlling what the kids eat when they are playing out there. They may eat sweets or other things they’re not supposed to eat; it stresses me at times.”

Fatuma says she was well trained by MSF prior to being given her own portable cooling box and insulin for her children. She understands what each reading means and what to do in each instance.
Ali Bishar Adan, in charge of MSF’s home-based insulin management programme, says Abdi was the first patient to be enrolled into the programme. “He is our patient number 001 under the programme and the mother has been one of the best,” he says.
Fatuma says the only challenge associated with the cooling box is that rats sometimes chew it, and scorpions and other small insects crawl inside to keep cool in Dadaab’s hot climate. But she cleans the box frequently and has learnt to hang it in a place where the insects cannot easily reach it.
For Fatuma, the biggest challenge is getting hold of enough food so that she can feed the children to coincide with their injections. “I inject each of them twice a day: in the morning and in the evening,” she says. “With every injection, the children need to eat. If we were to inject more frequently, where would I get the food to give them? I don’t have a job, and the food ration we are given by WFP is hardly enough for seven days.”
The younger boy experiences hypoglycaemia at least twice a week and sometimes more frequently, especially at night. “He does not eat well,” says Fatuma. “I try to force him to eat but he will not eat much. So I usually keep some food in a cooking pot or some milk to give him at night. I used to give them sweets and biscuits, but their teeth started decaying, so I stopped.”








